
Uniform fitted. Induction complete. 10-mission milestone reached. It has been a learning frenzy.
I’m a UK-trained emergency physician, and am two months into my year as a Sydney HEMS registrar. Some of my early reflections on the experience have had time to crystallise into bloggable form…
I’m one half of a tag team
Shared leadership has been a consistent theme. The doctor and critical care paramedic that make up a HEMS team both dictate the pace and direction at different phases of the mission. No “team leader” exists, it’s a tag team approach. This is an interesting contrast to the leadership model followed in the hospital environment and taught on life support courses, where there is always a singular team leader planted at the end of the bed, dictating proceedings with their gloves off.
Diplomacy skills are key
The nature of prehospital and retrieval medicine is there is almost always another team with the patient prior to your arrival. It might be a team of NSW ambulance paramedics first on scene at a motor vehicle accident, or the ED resus team knee-deep in managing a septic shock patient at a small regional hospital with no ICU. A crucial step is to carefully read the dynamics of the team already in place and integrate harmoniously. This might involve trusting the existing team leader and providing support as opposed to immediately seeking to supersede. It also might mean intervening on an unsafe situation for the patient and gently guiding the team in the right direction without provoking hostility. Diplomacy skills are key – we must “capture hearts and minds” to deliver efficient, quality care.
A collaborative, inclusive and sensitive approach was heavily emphasised throughout induction. We should arrive with a “friendly, skilled and here to assist where needed” attitude as opposed to “we’re the most qualified and now we’re calling the shots”. Interestingly, this mantra is (arguably) entirely at-odds with the bullish, uber-alpha persona that HEMS teams often get labelled with.
It’s hands (back) on
As the years have passed in my emergency medicine training, I spend less time physically examining patients. I think this is multifactorial: My experience now affords me a “leaner” assessment process (I’m better at only examining the anatomy I need to); my clinical supervision and non-clinical responsibilities increasingly remove me from the shop-floor; when I am working clinically, I spend more time in the “Early Senior Assessment” (i.e. senior decision-maker in triage) area where targeted history-taking is generally higher yield in those precious few minutes with the patient. With trauma patients in resus, I used to do the primary survey, now I’m the Trauma Team Leader – end of the bed, gloves off.
With HEMS, my hands must get back on the patient. My average patient will be sicker, surrounded by unfamiliar obstacles, and have dual pathology – disease process and geographical location. Time will be more critical (for my average patient), and my interventions will frequently be procedural. It is critical that anything we do to the patient is meaningful and justifiable. I’ll always have my experienced CCP teammate to request a sense-check from, but ultimately the clinical decision-making responsibility lies with me. It would be foolish (and negligent) to abbreviate or delegate the physical examination process.
Work smartly and add value
Throughout my training I’ve held the belief that the most important attribute of an ED doctor was to be a hard worker. I’ve been conditioned by the UK emergency medicine landscape where, regardless of season or time of day, it has become the norm for the waiting room to be bursting at the seams, and for the medical and nursing rota to contain countless unfilled shifts. This burnout-prone workplace has only been intensified multi-fold by the pandemic. The prevailing attitude tends to be:
Everyone on-shift needs to be flat out for us to survive the next 10 hours. We can worry about effectiveness later… if we get to it.
The problem with “work hard” being your central ideology is that it is non-specific. There are loads of different ways to work hard as an emergency physician. The application of effort is dictated by a range of variables: current wait-time, who else is on shift, junior to senior ratios, unexpected teaching opportunities, bed availability, number of “sickies” (properly unwell patients), and personal preference (i.e. what does one enjoy the most when on the shop-floor), among others. Two emergency physicians with contrasting personalities and interests will interpret how best to add value to the same shift in completely different ways. Working hard, but not necessarily working smart.
There is beautiful simplicity in a doctor-CCP team that (usually) sees one patient at a time. There are fewer moving parts, and the goalposts are clearer. Furthermore, there are limited options in terms of “doing stuff” as work activities orbit individual patients, of which there are far fewer compared to your average ED shift. This makes the process of unpacking the individual components of the job less burdensome, and the pursuit of high performance more intuitive.
Essentially, there is a clear roadmap for how and where to apply effort. And it hinges on the doctor and CCP understanding precisely what their job is, but equally, what their job isn’t. No ambiguity. As the doctor my role is to provide advanced clinical oversight and a critical care procedural skillset. The CCP leads on scene management, logistics, and patient handling. There should be minimal task overlap, but a deep understanding and awareness of each other’s role and task-list.
Both of us should know what our individual objectives are, and the specific value we are adding to team performance.
The best HEMS teams are “implicitly co-ordinated”
Whilst an elite-level doctor-CCP team will understand their individual value and stay in their respective lanes as described above, they will always be anticipating (and therefore helping to facilitate) their teammate’s next move. Minimal prompting. Perfect choreography.
The journey to this “implicit co-ordination” starts with interdisciplinary cross-training during induction. Both groups received essentially identical training, other than the sims where we participated in our usual job roles. This exposure to the CCP role meant regular deep dives into the practical aspects of prehospital and retrieval medicine. We were trained in how to make things happen.
The truth is I found this element of induction confronting. The practicalities of critical care feel a great deal further from my comfort zone than the decision-making. I’ve tended to rely heavily on resus nursing staff to carry out the fundamental processes needed to manage sick patients. Too often I’ve strategically used my position as team leader to dodge getting my hands dirty – knowing deep down that I would likely fail to complete key practical tasks if I were to attempt them. My ability to make things happen has been embarrassingly limited. A top priority this year for me will be turning this weakness into a strength.
I still feel at the beginning of my journey to high performance in this component of the game, but with one-on-one coaching from world class CCP colleagues on every shift I can see my path forwards lit brightly. What a gift.
Important new concept – “workflow”
I often find the most powerful educational experiences are when an expert drills right down into the granular detail of his/her process.
“You rest your hypothenar eminence on the patient in an overhand grip and stabilise the insertion needle.”
“I start reading my putt when I’m walking up the fairway, as I get a better appreciation of the green undulations on the approach.”
“I say the exact words ‘you have control’ when handing over the controls of the aircraft to the First Officer. The same three words every time.”
At the Royal London Hospital last year my most memorable training moment came when a phenomenal Trauma Team Leader (and mentor) walked me through each micro-step of orchestrating a trauma patient off the scoop stretcher prior to the commencement of the primary survey. From positioning of trauma team personnel to the precise verbal commands when bracing the patient. On the surface a routine, uncomplicated, and non-crucial process. However, if done with authority and fluidity it sets a professional and confident tone for the resuscitation, commands the respect of your trauma team, and ultimately fosters better “followership”. If done poorly, it can rapidly delete your credibility as a leader.
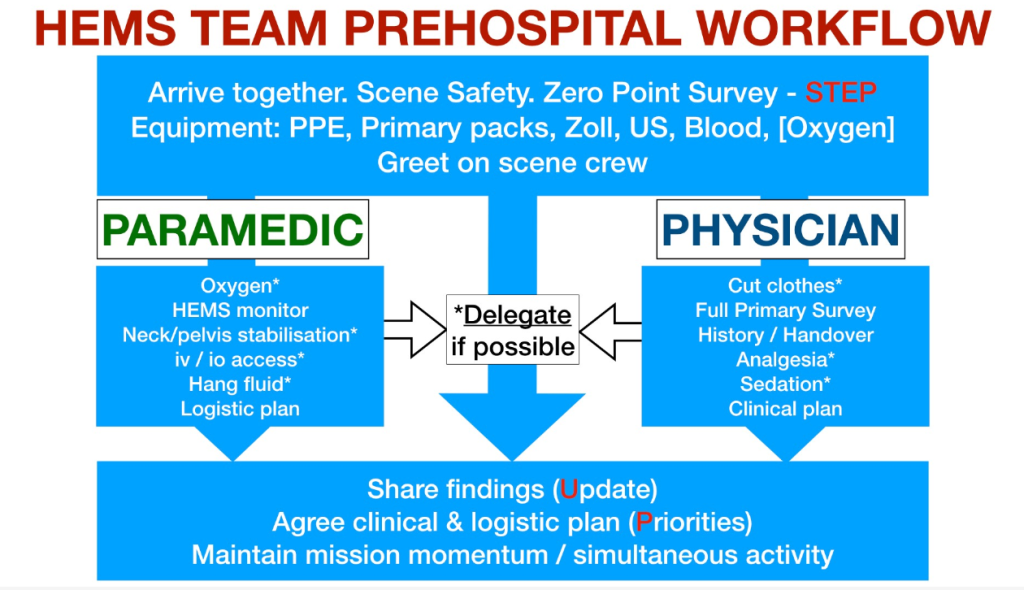
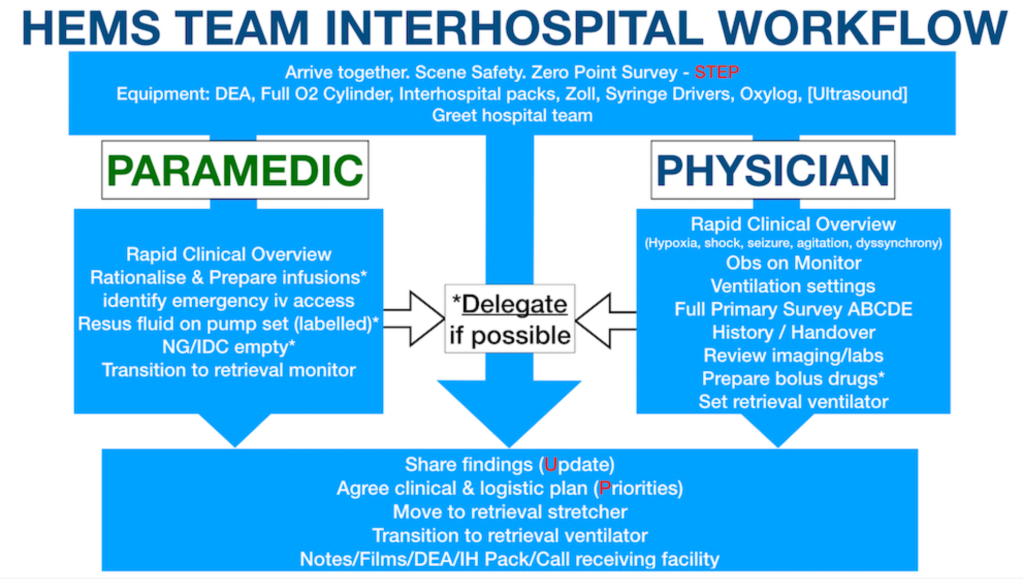
I found a similarly illuminating experience when the induction faculty unpacked each micro-step of the HEMS “workflow”.
A wonderful feature of all prehospital/interhospital missions is the time taken to get to the patient doubles up as an opportunity for relatively uninterrupted planning, syncing up of mental models, and mental rehearsal.
On arrival, the handover is taken together, before the team divide and conquer their role-specific objectives. Other capable healthcare providers on-scene should be assigned appropriate clinical jobs to preserve the team’s mental bandwidth and situational awareness. The team should come back together at regular interval to re-sync mental models, establish priorities and plot next steps.
This game-plan, at its core, should be identical every mission.
Am I sharing my mental model… or verbal diarrhoea?
When I’m feeling under pressure I talk too much. It’s a nervous tick. As I’ve gained more experience and professional confidence over the years, it’s become less of an issue. I can usually spot it early and proceed to consciously improve the signal-to-noise ratio of my own vocal contributions. However, the further I get from my comfort zone, the more it creeps back.
I was very nervous in the induction simulations. They were epic in scope, expertly facilitated, and full of purpose. I, like everyone else, was desperate to put my best foot forward in front of new colleagues. Feedback I received on more than one occasion in sim debriefs was I shared my mental model so regularly that it impeded my CCP colleague from getting things done. I kept interrupting their flow, which stifled our momentum as a team.
It was the most heightened physiologically I had felt in a training exercise in as long as I can remember. The result was a failure to self-police my destructive babbling.
Of course, one’s mental model must be shared where appropriate, but verbal diarrhoea has to be avoided when time is critical. Communications must be meaningful (just like our interventions). This has been a hugely important point of reflection for me personally, and one that I have thought about en route to all my missions so far.
Robbie Lloyd
Sydney HEMS registrar
@Ponder_Med

You can find more reflective lessons from Sydney HEMS over at St Emlyn‘s

Great post mate!
Pingback: Reflecting on two months as a Sydney HEMS registrar – Wound Care News